Open book fracture rehabilitation training and exercise for patient for young age
- Dhivakar A
- Jul 26, 2025
- 3 min read
Here’s a detailed guide for open‑book pelvic (anteroposterior compression, APC II/III) fracture rehabilitation in a young patient, including pre- and post-operative exercise protocols. The image above illustrates the nature of an open‑book injury where the pubic symphysis separates, resembling an opening book (Wikipedia).
🛡️ Injury Overview
An open‑book pelvic fracture occurs from an anterior–posterior force causing the pelvis to externally rotate and separate at the pubic symphysis; posterior ligaments (such as sacroiliac ligaments) may also be disrupted in more severe cases (Wikipedia, Wikipedia).
Treatment often involves surgical fixation (e.g., plating of the symphysis and/or iliosacral screws) followed by tailored rehabilitation depending on stability and fixation method (surgeryreference.aofoundation.org).
🩺 Rehab Approach: Pre- and Post‑Surgery Phases
Pre‑operative (If surgery is delayed)
Pain and swelling control: Pelvic binder, RICE, minimize movement.
Bed mobility and breathing exercises: Frequent position changes to prevent pulmonary complications and skin breakdown (PMC, surgeryreference.aofoundation.org).
Gentle mobility: Ankle pumps, isometric glutes/quads, toe/knee/hip active–assisted ROM.
Strength maintenance: Core and upper‑body isometrics; non‑involved side strengthening.
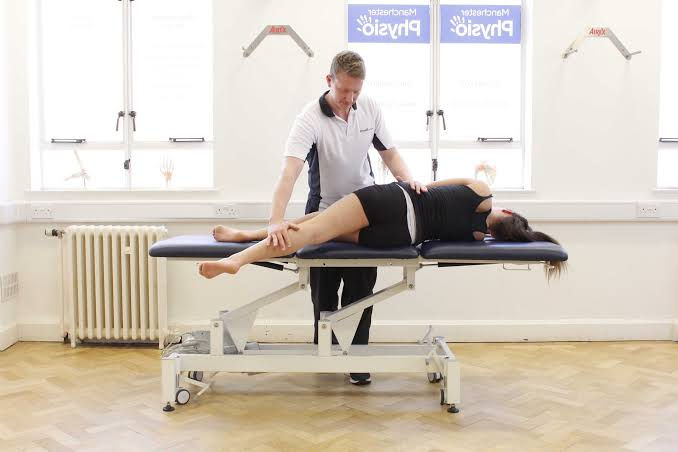
Early Post‑Op (Days 1–14)
Start bed-to-chair transfers, often with a sliding board, the day of or soon after surgery (articulate., TeachMe Orthopedics).
Respiratory physiotherapy, ankle pumps, and deep breathing to reduce risk of DVT and lung complications (PMC, surgeryreference.aofoundation.org).
Isometric exercises: glutes, quads, hamstrings. Gentle active-assisted upper/lower limb ROM.
Touchdown weight-bearing (just the foot) for unilateral injuries as advised by surgeon (surgeryreference.aofoundation.org).
Sample early exercises:
Ankle pumps: 20 reps hourly to improve circulation (Cambridge University Hospitals).
Heel slides (knee/hip ROM): 10 reps, 3–4 times/day (Cambridge University Hospitals).
Static quads and glute squeezes: hold 5–10 s, 10 reps, 3–4 times/day (Cambridge University Hospitals).
Pelvic tilts and glute bridges for core control and pelvis stability (PMC, In Motion O.C. -).
Intermediate Phase (Weeks 2–6)
Progress weight-bearing: From touchdown → partial weight-bearing (PWB) at 6 weeks, per radiographic/healing status (articulate.).
Introduce assisted ROM for hip, knee, and ankle.
Begin active exercises like bridges, heel slides, leg abductions/adductions, core activation (clamshells, tabletop) (Cambridge University Hospitals, forum.facmedicine.com).
Rehabilitation Phase (Weeks 6–12)
As bone and ligament stability improves:
Increase PWB, slowly transitioning to full weight-bearing by ~12 weeks as tolerated and imaging permits (surgeryreference.aofoundation.org, articulate.).
Strength training:
Mini squats, hip flexion/extension, bridges with progressions, clamshells with band,
Resisted hip abduction/adduction, gentle bike or stationary pedaling to boost mobility and circulation (forum.facmedicine.com).
Balance and gait: walking frame/crutch-assisted gait training, static single-leg balance exercises.
Advanced Phase (3–6 months & beyond)
Transition to functional activities and controlled-impact exercises.
Core strengthening: planks, side planks.
Dynamic lower limb conditioning: lunges, side monster walks, resisted band drills, single-leg hops as tolerated (surgeryreference.aofoundation.org, Reddit).
Sport-specific training or return to high‑level activities gradually, if appropriate and cleared.
📋 Summary Table
PhaseWeight

BearingExercises FocusPre‑Op & Early Post‑OpBed‑mobility; touchdown or noneAnkle pumps, heel slides, isometricsWeeks 2–6Partial weight-bearing (PWB)Glute bridges, core activation, leg mobilitiesWeeks 6–12Progress to full weight-bearingMini squats, resisted hip work, balance training3–6 Months+Full activities as toleratedDynamic drills, functional & sport prep
⚠️ Precautions & Guidance
Always follow surgeon’s allowed weight-bearing limits and healing status: radiographic monitoring required (typically every 4–6 weeks) (surgeryreference.aofoundation.org, articulate., Musculoskeletal Key).
Avoid high-impact or twisting movements until bone healing is confirmed.
Monitor for complications: infection, nerve injury, DVT, hardware irritation, pelvic asymmetry, or gait deviations.
✅ Tips for a Young Patient
Encourage strong core engagement and focus on pelvic floor activation.
Use aquatic therapy when available: gentle aquatic walking or resistance movement can help early functional progression (Champion Performance & Physical Therapy).
Incorporate progressive band resistance, bodyweight functional training, and plyometrics as balancing, strength, and pain permit.
Tailor rehab to activity level: more aggressive progression is possible if healing is confirmed and surgeon agrees.
Would you like a personalized weekly rehab schedule or sample videos for specific exercises? Let me know!



Comments